News
17 April 2024
Home Slider
K18 – the Key to Unlocking Informed Decisions in MASH Drug Trials
Join us for an enlightening webinar presented by Jessica Tuohy, a distinguished partner and colleague from the US, focusing on the significance of K18 as a biomarker in the development of treatments for MASH (Metabolic Associated Steatohepatitis). This webinar is essential for drug developers, doctors, researchers, and key opinion leaders in the field of metabolic liver diseases, offering deep insights and key research findings.
Event Details:
- Date: Tuesday, April 23
- Time: [1pm EDT, 7pm CET]
Webinar Overview: This session will cover several critical areas:
- – An Introduction to the Growing Epidemic of MASLD (Metabolic Associated Steatotic Liver Disease)
- – Challenges in Developing Therapies for the Treatment of MASH
- – An Overview of K18 and Its Role in MASH Pathogenesis
- – A Review of Data That Support the Value of K18 as a Biomarker for Assessing the Efficacy of Drug Candidates in MASH Clinical Trials
Who Should Attend:
- – Drug developers in the field of MASLD and MASH.
- – Physicians and healthcare professionals specializing in hepatology, gastroenterology, and related fields.
- – Medical researchers focusing on liver disease and drug development.
- – Key opinion leaders in metabolic liver diseases.
Registration: Please register here to secure your spot in this informative webinar. Registration is required to access this online event.
Additional Information: If you are unable to attend the live event, a recording will be made available to all registered participants, ensuring you can access this webinar at your convenience.
We look forward to welcoming you to what promises to be an informative and transformative session.
For more information, please contact us at marketing@vlvbio.com.
Don’t miss out on the chance to advance your knowledge in MASH treatment and diagnostics. Reserve your spot today!
23 January 2024
Blog
Launch of IMMUNIS Cytokeratin 18F EIA by Institute of Immunology, Japan
We are thrilled to share a momentous achievement in our longstanding collaboration with our esteemed Japanese partners, the Institute of Immunology. This announcement comes during a meeting filled with collaboration and shared successes as Mr. Ito, Mr. Akira, and Ms. Yukiko from the Institute of Immunology paid a visit to our headquarters in Stockholm.
During this collaborative visit, we had the pleasure of discussing plans for the imminent launch of the IMMUNIS Cytokeratin 18F EIA, a project that holds significant promise in the realm of diagnostic medicine. This project has been a work of dedication and innovation, and the collaboration between VLVbio and the Institute of Immunology has been instrumental in its success!
We are happy that the IMMUNIS Cytokeratin 18F EIA has gained official approval as an In Vitro Diagnostic (IVD) for the diagnosis of Non-Alcoholic Steatohepatitis (NASH) from the Pharmaceuticals and Medical Devices Agency (PMDA) in Japan! This recognition underscores the product’s efficacy and reliability in contributing to the diagnosis and management of NASH, a condition of growing concern globaly as the epidemiology of the disease keeps increasing at an alarming rate. The need for a biomarker to identify patients with NASH and who are at risk of significant liver disease is of utmost importance, and we are happy that the Keratin 18 assay can assist in that!
The IMMUNIS Cytokeratin 18F EIA ELISA kit
Of equal importance, the IMMUNIS Cytokeratin 18F EIA, developed by the Institute of Immunology, has been included in the national health insurance system in Japan. This recognition ensures widespread accessibility, facilitating broader usage of this diagnostic tool within the Japanese healthcare community.
We are pleased to announce that the official launch date for the IMMUNIS Cytokeratin 18F EIA is scheduled for February 26th to the Japanese market. This date signifies the conclusion of a meticulous research and development process and exemplifies the collaborative efforts between VLVbio and our esteemed partners at the Institute of Immunology. The IMMUNIS Cytokeratin 18F EIA, launched by the Institute of Immunology, is poised to make a substantial impact on the field of NASH diagnosis, providing healthcare professionals with an additional tool to enhance their diagnostic capabilities in Japan.
As we celebrate this milestone and the successful visit from our partners, we extend our gratitude to all individuals who have contributed to the realization of this project, including the dedicated team members and esteemed partners at the Institute of Immunology. Congratulations to you all!

Institute of Immunology president Mr. Ito Yukio and VLVbio CEO
Mrs. Slavica Brnjic holding the finished IMMUNIS Cytokeratin 18F assay.
9 April 2026
Blog
Monitoring MASLD: Why Assessing Treatment Response Remains a Clinical Challenge
Metabolic Associated Steatotic Liver Disease (MASLD) is increasingly recognized as a major global health concern, closely linked to metabolic conditions such as obesity and Type 2 diabetes. While awareness and diagnostic capabilities have improved in recent years, managing MASLD remains challenging, particularly when it comes to assessing treatment response over time.
With the therapeutic landscape evolving, including the introduction of pharmacological treatments alongside established lifestyle interventions, clinicians are now faced with an important question: how can we reliably monitor whether a patient is improving?
The Challenge of a Silent and Dynamic Disease
MASLD often progresses without clear symptoms, especially in its early and intermediate stages. Patients may feel well even as underlying liver injury continues. This disconnect makes objective monitoring tools essential, particularly when evaluating the effectiveness of treatment.
At the same time, MASLD is not a static condition. Disease activity can fluctuate depending on metabolic control, weight changes, or therapeutic interventions. As a result, clinicians require tools that can capture ongoing biological processes, rather than relying solely on static or structural assessments.
Limitations of Current Monitoring Approaches
Liver Enzymes (ALT, AST)
Liver enzymes are widely used in clinical practice but have important limitations. Many patients with MASLD may present with normal ALT and AST levels despite ongoing liver injury, while others may show fluctuations that do not reflect meaningful histological changes. As such, liver enzymes alone are often insufficient to monitor treatment response.
Imaging Techniques
Non-invasive imaging tools, such as ultrasound or elastography, provide valuable information about liver fat and fibrosis. However, these methods primarily assess structural changes and may not capture early or dynamic changes in disease activity, particularly in response to short-term interventions.
Liver Biopsy
Liver biopsy remains the reference standard for assessing disease activity and fibrosis. However, its use in routine follow-up is limited due to:
- – Invasiveness and patient burden
- – Sampling variability
- – Cost and logistical constraints
For these reasons, repeated biopsies are not practical for monitoring treatment response in most patients.
A Growing Need in the Era of MASLD Treatment
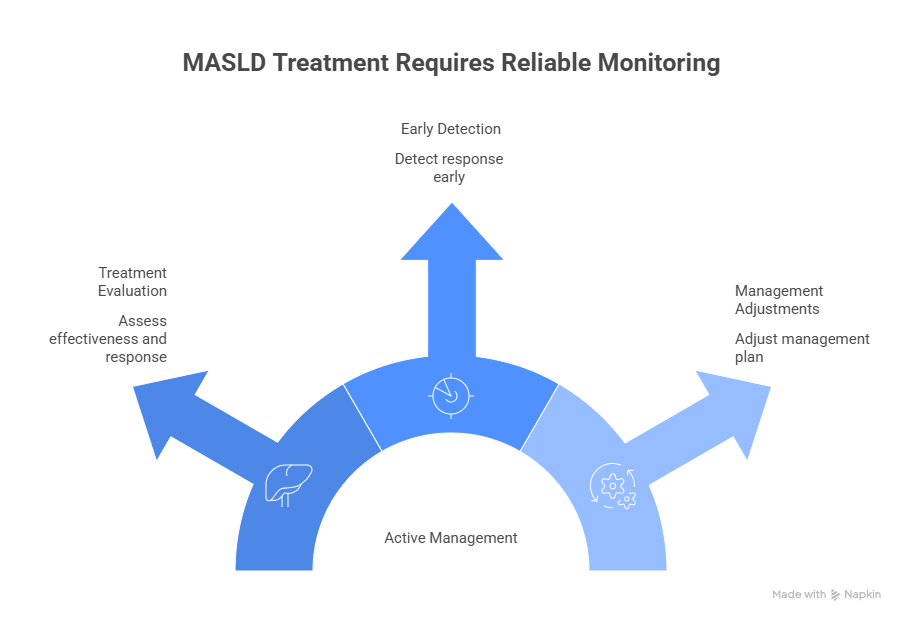
The need for reliable monitoring tools has become even more pressing as MASLD enters a new phase of active management. With the development of pharmacological therapies, alongside lifestyle and surgical interventions, clinicians must now evaluate:
- – Whether a treatment is effective
- – How early a response can be detected
- – Which patients may require adjustments in their management plan
This shift highlights a clear gap in current clinical practice: the lack of accessible, non-invasive tools that reflect ongoing liver injury and response to therapy.
Moving Toward Biological Markers of Disease Activity
To address these challenges, attention will increasingly turn toward biomarkers that reflect underlying disease mechanisms, rather than only structural liver changes.
One such mechanism is hepatocyte apoptosis, a key feature of MASLD progression, particularly in metabolic dysfunction-associated steatohepatitis (MASH). Measuring this process may provide a more direct insight into active liver injury and how it changes over time.
Biomarkers targeting apoptosis, such as those detecting fragments of keratin-18, have therefore been explored as tools to support treatment monitoring and improve clinical decision-making.
Looking Ahead
As MASLD management continues to evolve, the ability to monitor treatment response accurately and non-invasively will be critical. Understanding how different tools reflect disease activity, and how they can be integrated into clinical practice, will play a central role in improving patient outcomes.
In the next post in this series, we will explore how treatment monitoring is becoming increasingly important in the context of emerging pharmacological therapies, and how biomarkers are being used in clinical trials to assess response.
30 April 2026
Blog
Monitoring MASLD: Assessing Response to Pharmacological Treatment
The therapeutic landscape of MASLD is undergoing a fundamental shift. With the recent approval of resmetirom (Rezdiffra™) and the continued development of agents such as GLP-1 receptor agonists, MASLD is moving from a condition managed primarily through lifestyle intervention to one increasingly treated with targeted pharmacological therapies.
This transition introduces a critical question:
“How can treatment response be assessed in a disease where clinical symptoms are limited and traditional biomarkers are poorly aligned with underlying pathology?”
Mechanistic Complexity of Treatment Response in MASLD
MASLD is not a single-pathway disease. It is characterized by a complex interplay of:
- – Hepatic lipid accumulation (steatosis)
- – Insulin resistance and metabolic dysregulation
- – Inflammatory signaling
- – Hepatocyte injury and apoptosis
- – Fibrogenesis and extracellular matrix remodeling
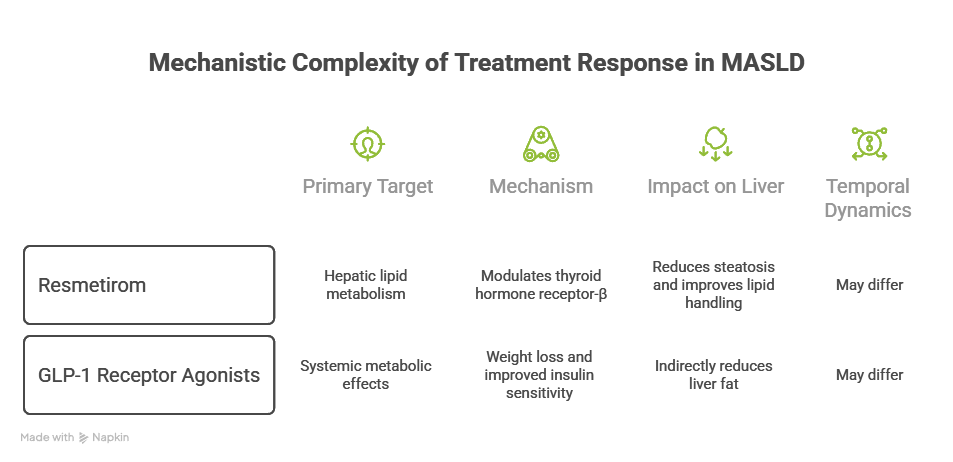
Pharmacological therapies target different aspects of this spectrum. Resmetirom (a thyroid hormone receptor-β agonist) primarily modulates hepatic lipid metabolism, reducing steatosis and improving lipid handling. In contrast, GLP-1 receptor agonists such as semaglutide exert systemic metabolic effects, including weight loss and improved insulin sensitivity, leading indirectly to reductions in liver fat.
While these therapies may ultimately converge on improving liver histology, their mechanisms of action differ, and so too may the temporal dynamics of response.
Limitations of Conventional Monitoring Endpoints
Biochemical Markers
Serum transaminases (ALT, AST) are widely used in clinical practice but have well-documented limitations. They lack sensitivity for detecting ongoing hepatocyte injury, and changes in ALT may not correlate with histological improvement, particularly in patients with advanced fibrosis. In addition, normal ALT levels are frequently observed in patients with active MASH.
Imaging-Based Assessments
Imaging modalities such as MRI-PDFF and elastography provide valuable information on hepatic fat content and liver stiffness as a proxy for fibrosis. However, reductions in liver fat do not necessarily reflect resolution of inflammation or hepatocyte injury. Furthermore, fibrosis regression is typically slow, limiting the utility of these tools as early treatment endpoints.
Histological Endpoints
Liver biopsy remains the reference standard in clinical trials, enabling assessment of steatohepatitis resolution and fibrosis stage. However, biopsy is constrained by sampling variability and Invasiveness and is hence impractical for real world serial monitoring
A Gap Between Treatment and Decision-Making
While pharmacological treatment options are expanding, clinical frameworks for monitoring and decision-making remain under development. In routine practice, questions such as:
- – When should a therapy be considered ineffective?
- – When should treatment be escalated or switched?
- – What constitutes a meaningful response?
are not yet clearly defined in current guidelines.
This creates a disconnect between the availability of therapies and the ability to act on treatment response, highlighting the need for monitoring approaches that can provide more informative and dynamic insights into disease activity.
Biomarkers in Clinical Trials: Capturing Dynamic Disease Activity
Given these limitations, there has been increasing interest in circulating biomarkers that reflect active disease processes, particularly in early-phase treatment response.
One of the key pathological features of MASLD progression, especially in MASH, is hepatocyte apoptosis. This process contributes directly to inflammatory signalling, activation of stellate cells, and fibrogenesis.
Fragments of caspase-cleaved keratin-18, released during apoptosis, can be detected in circulation and quantified using assays such as M30 Apoptosense® ELISA.
M30® in Pharmacological Studies
M30® has been incorporated into multiple MASLD clinical studies as a non-invasive biomarker of hepatocyte injury and treatment response.
- – Reductions in M30® levels have been associated with improvements in histological features of disease activity, including ballooning and inflammation (Davison et al., Journal of Hepatology, 2021).
- – In interventional settings, M30® has demonstrated responsiveness to therapeutic modulation, reflecting reductions in apoptotic activity in parallel with metabolic and histological improvements.
Importantly, M30® captures a dimension of disease activity that is not directly assessed by imaging or standard biochemical tests; the rate of ongoing hepatocyte injury.
Temporal Aspects of Treatment Response
One of the key advantages of biomarkers reflecting apoptosis is their ability to detect early biological changes.
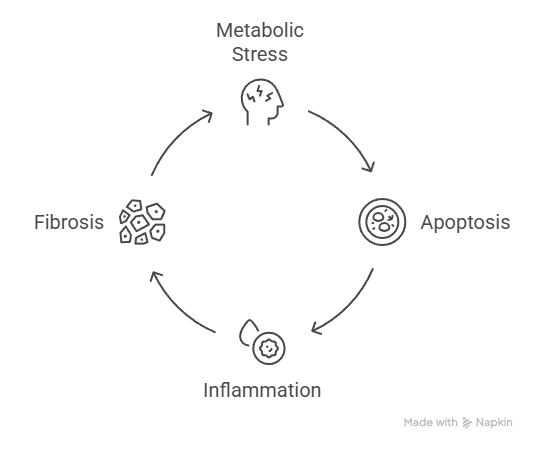
Pharmacological interventions may rapidly influence lipid metabolism or insulin sensitivity, but the downstream effects on inflammation and fibrosis may take longer to manifest. Apoptosis sits at an intermediate point in this cascade, downstream of metabolic stress but upstream of fibrosis, making it a potentially sensitive marker of early response.
This positions biomarkers such as M30® as useful for:
- – Early signal detection in clinical trials
- – Assessing biological response before structural changes become evident
Toward Integrated Monitoring Strategies
No single marker fully captures the complexity of MASLD. Instead, a multi-modal approach is likely required, combining structural assessment (imaging and fibrosis scores), functional markers (liver enzymes), and mechanistic biomarkers such as apoptosis markers.
Within this framework, M30® can provide insight into ongoing hepatocyte injury, complementing other tools that assess steatosis or fibrosis.
Looking Ahead
As pharmacological therapies become more widely used in MASLD, the need for sensitive, non-invasive, and mechanistically relevant biomarkers will continue to grow.
Beyond detection, future monitoring strategies may also need to support clinical decision-making, helping to identify non-responders and guide therapeutic adjustments, areas where current guidance remains limited.
In the next post in this series, we will explore in more detail the biological role of hepatocyte apoptosis in MASLD, and why it represents a key target for both disease understanding and monitoring.
11 December 2025
Home Slider
Thank you for being part of our 2025
Dear colleagues, partners, and friends,
As we conclude another remarkable year, we want to extend our sincere gratitude to each of you; our distributors, collaborators, and partners around the world.
2024–2025 has been a year defined by progress, dialogue, and renewed momentum in the MASLD/MASH field. We are truly grateful for the continued trust, engaged discussions, new scientific contacts, and the many constructive conversations we’ve shared with you throughout the year.
The global MASLD landscape is evolving faster than ever. The release of Rezdiffra™ in the United States has already brought meaningful benefit to many patients, marking a long-awaited step forward in treatment availability. With the recent approval in Europe, we are excited to see this progress finally reach European patients, which is a milestone the field has been anticipating for decades.
Likewise, the approval of semaglutide for MASH adds an important therapeutic option. After years of limited tools, we are now entering a new phase where patients with MASH can finally receive the help they need.
But as treatment availability expands, a new challenge has emerged:
How do we effectively monitor patients on therapy?
This question has been raised repeatedly in our conversations with clinicians, KOLs, and partners this year, and it is becoming one of the central needs in clinical practice.
In this evolving landscape, M30 Apoptosense® ELISA has shown clear potential to fill an important part of this gap.
Evidence from multiple clinical trials, including Madrigal’s phase III MAESTRO-NASH trial, has shown that M30® (ccK18) is one of the leading blood-based indicators of treatment response, outperforming several structural NITs in early prediction of change. Importantly, M30® offers:
- – Early, biology-based insight into hepatocellular injury
- – Reliable tracking of treatment effect before structural changes become visible
- – A practical solution for clinics without access to advanced imaging such as MRI-PDFF
- – A low-cost, accessible assay that integrates easily into routine follow-up workflows
As more patients in the US and Europe begin therapy, the need for simple, repeatable, blood-based monitoring tools has never been clearer. We are proud that our M30 Apoptosense® ELISA continues to serve as a scientifically grounded, widely studied option to support clinicians and improve real-world treatment follow-up.
Looking ahead to 2026, we are excited to continue supporting you; through scientific collaboration, distributor partnerships, educational materials, and tools that strengthen your local markets. Your work is essential for bringing knowledge, clarity, and better care to patients worldwide, and we value the role you play in this shared mission.
From all of us at VLVbio:
Thank you for a productive, inspiring, and forward-moving year.
We look forward to continuing our work in 2026.
The VLVbio Team

12 June 2025
Home Slider
Global Fatty Liver Day
1 in 3 adults has fatty liver disease. And many don’t even know it.
Today on Global Fatty Liver Day, we stand with the global health community to raise awareness of this silent epidemic and the power of early detection.
At VLVbio, we’re committed to supporting healthcare professionals with diagnostic tools that enable timely action. Read more on how the VLVbio products assist diagnosing steatotic liver diseases here!
Know it. Test it. Treat it. 💚
22 May 2025
Home Slider
Play For Your Liver
Liver disease isn’t just an adult problem.
Today, 1 in 10 children are at risk of MASLD (Metabolic dysfunction-associated steatotic liver disease), and the numbers are rising fast.
At VLVbio, we believe that prevention starts young – through movement, healthy habits, and community support.
That’s why we’re proud to sponsor a local Swedish youth football team, promoting an active lifestyle and early liver health awareness.
Because every goal scored is a step toward a healthier future! ⚽
Watch our short campaign video below to see how we’re helping raise awareness and protect the next generation, one active child at a time.
#PlayForYourLiver
25 April 2025
Home Slider
The EASL Congress 2025
We are heading to Amsterdam for the EASL Congress together with the European Association for the Study of the Liver!
We’re happy to yet again be exhibiting at #EASLcongress with EASL | The Home of Hepatology! We are happy to yet again be an industry partner for the biggest liver event in Europe!
The latest in hepatology is happening 📅 7–9 May.
🤝 Join us at the highlight of the year! Register today, and lets meet and discuss liver biomarkers at our booth.
